About Age-related macular degeneration (AMD) and Geographic Atrophy (GA)
Age-related macular degeneration (AMD) is a progressive disease of the macula, which is the central part of the retina, and plays a key role in vision.1 AMD represents one of the most common causes of vision loss in Western industrialised countries. One quarter of Europeans over the age of 60 are affected by AMD, be it early, intermediate or late-stage AMD.2 This section discusses the different forms of advanced AMD, including geographic atrophy (GA).
How vision works
Light enters the eyes and passes into the retina, which lines the inner back of the eye. The retina has millions of photoreceptors (light-sensitive cells), which turn light into electrical signals. These signals travel to the brain via the optic nerve, allowing us to process what we see.3
Watch this video to explore how vision works in more detail.
The role of the macula and the effect of ageing
The macula is the name for the small area in the centre of the retina. It has the highest concentration of light-sensitive photoreceptors, which turn light into electric signals.3 The macula is the part of the eye that processes what you see directly in front of you – known as your central vision. It lets you see small details and focus on very specific aspects of what you’re looking at.4 For example, it helps you make out text on a page or the differences in faces.
Over the course of our lifetime, the macula is affected by the high-energy light that our eyes are constantly processing. As light enters the eye and is transmitted by the photoreceptors, waste products known as drusen are produced. Over time, drusen build up because the cells responsible for removing them can no longer do so quickly enough. The drusen build up under the macula, causing photoreceptors to degrade and die over time, which disrupts the visual process. When this occurs, it is known as age-related macular degeneration, or AMD.3,5
Most people are affected by early or intermediate AMD, but approximately 2% of those with AMD will go on to develop an advanced form of AMD, which is discussed in the following sections.
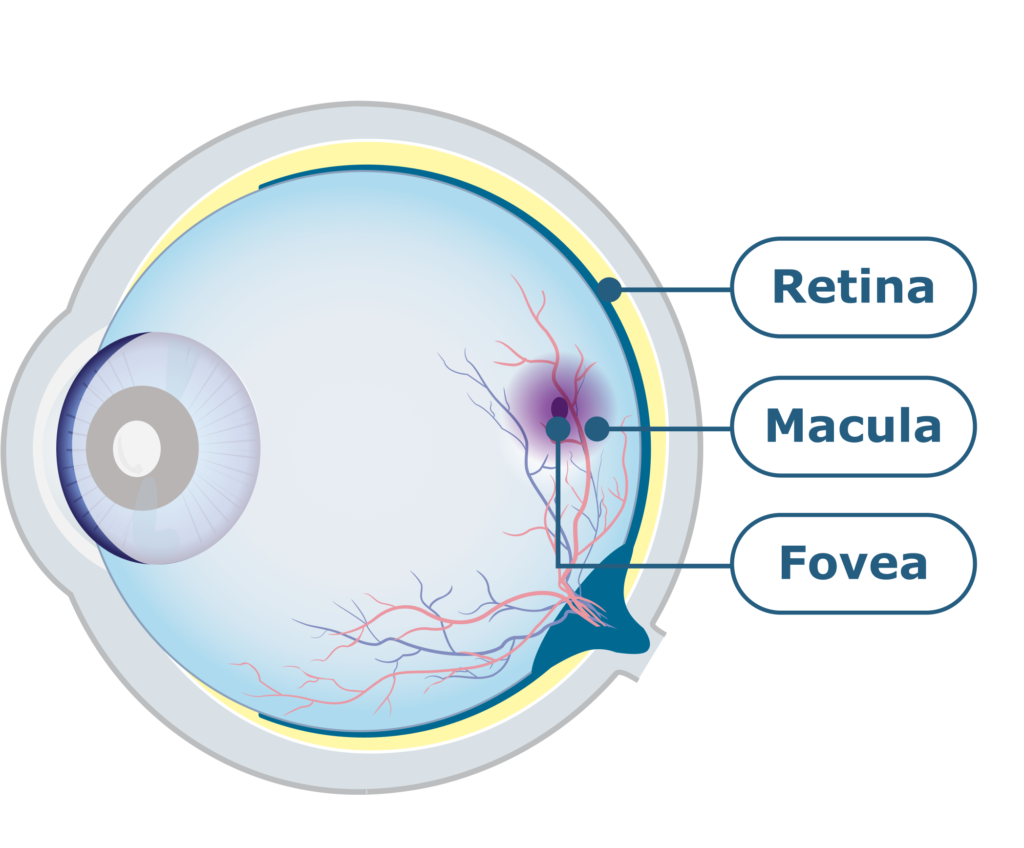
Cross-section of the eye.
Types of age-related macular degeneration
There are various eye disorders that affect the macula, and they are collectively referred to as ‘macular degeneration’. Since this eye disease mainly affects people over the age of 65, it is also called age-related macular degeneration, or AMD.6,7
There are two main types of this disease: wet and dry AMD. Wet AMD develops when abnormal blood vessels grow beneath the macula and damage it, whereas dry AMD involves the build-up of waste products, known as drusen, causing damage to the macula.3,6
Advanced age-related macular degeneration
Advanced AMD, which includes both dry and wet AMD, is considered to be the largest cause of vision loss in industrial nations.8 An eye with the advanced form of dry AMD can also naturally develop wet AMD, and vice versa.9
One of the advanced forms of AMD is known as geographic atrophy, or GA, which affects approximately 5 million people around the world.10 About 40% of advanced AMD cases are geographic atrophy, while 60% are wet AMD.2
Watch this video to learn more about the advanced forms of AMD.
Geographic atrophy
Geographic atrophy (GA) refers to an advanced form of AMD. It is characterised by the accumulation of small yellow deposits of fatty proteins, called drusen, under the retina and macula.11
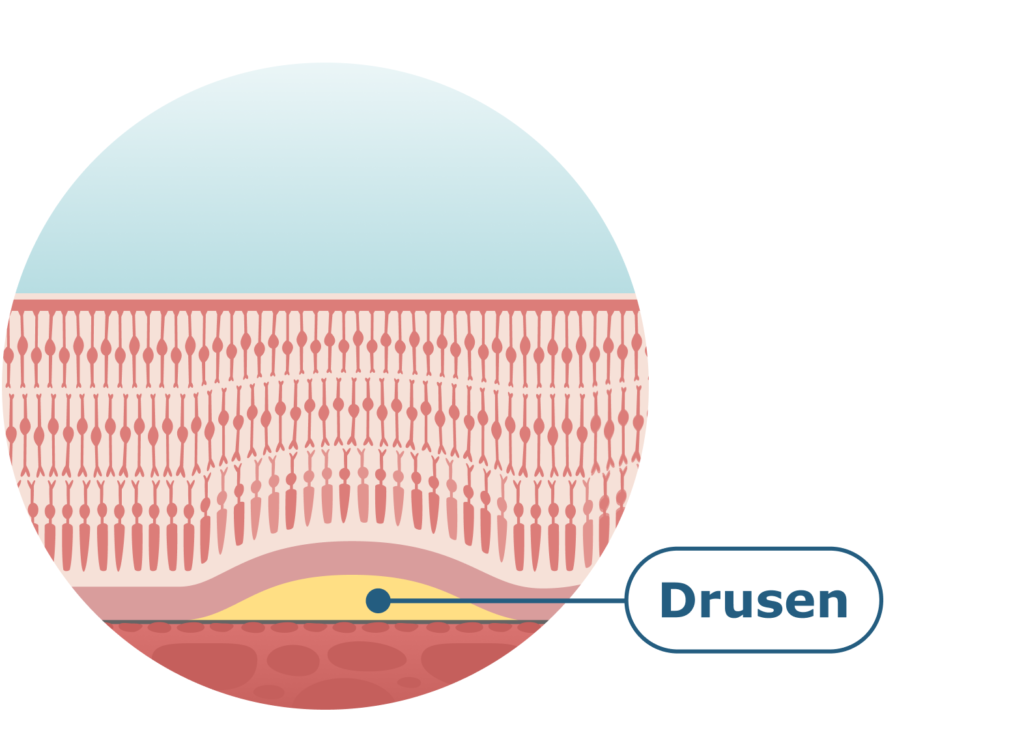
Cross-section of the macula.
In the early stage of AMD, a few small and medium-sized drusen can be detected in the eye. The intermediate stage is characterised by the presence of medium-sized drusen or one large one. When AMD reaches an advanced form, or GA, this is noted by the presence of more than one large drusen or drusen that merge together.
In GA, blind spots usually first appear outside of the central field of vision. As the disease progresses the central field of vision is affected, and this ultimately leads to vision loss. The name ‘geographic atrophy’ refers to areas of atrophy or damage, which may look like a map to the examining doctor, hence this term.12
The stages of geographic atrophy
While lesion growth in GA may appear to proceed slowly, disease progression is often constant and irreversible.13–16
Stages of GA progression16
Non-central atrophy
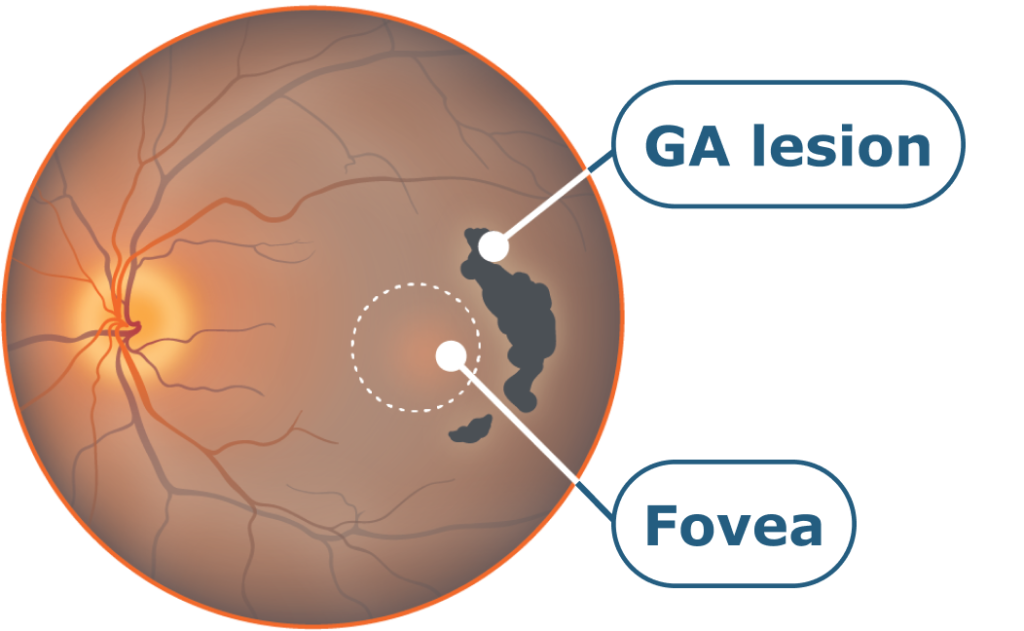
Some loss of peripheral low light vision. Patient only notes under certain conditions or through designed tests.
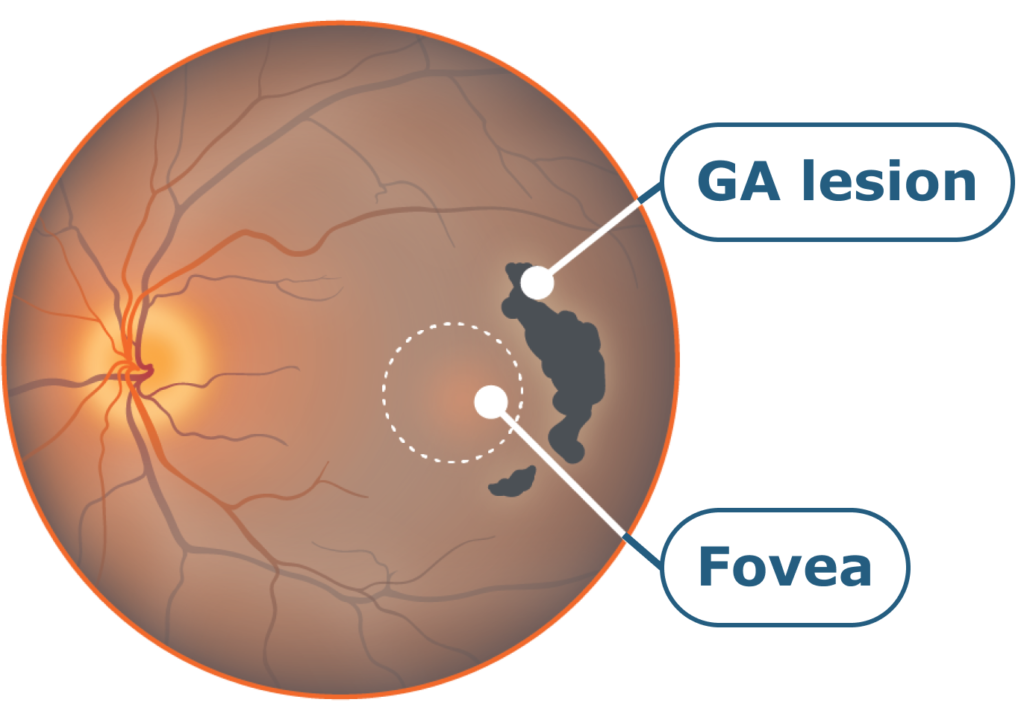
Growth of non-central atrophy
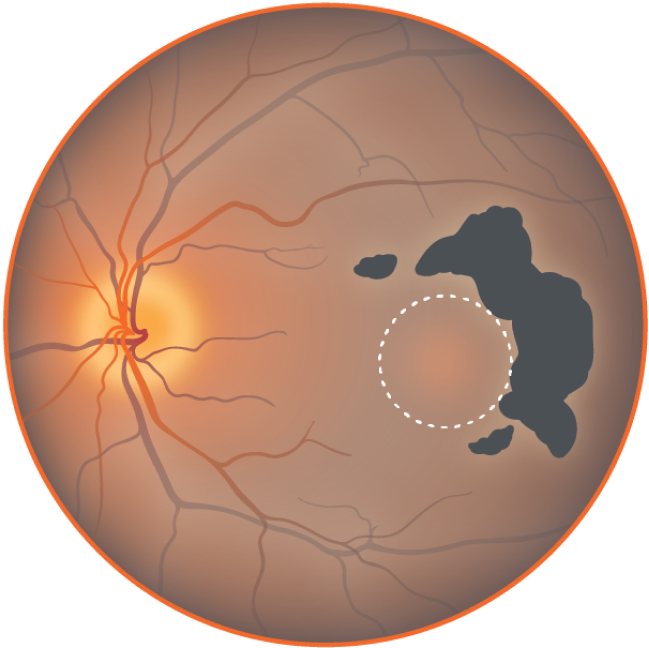
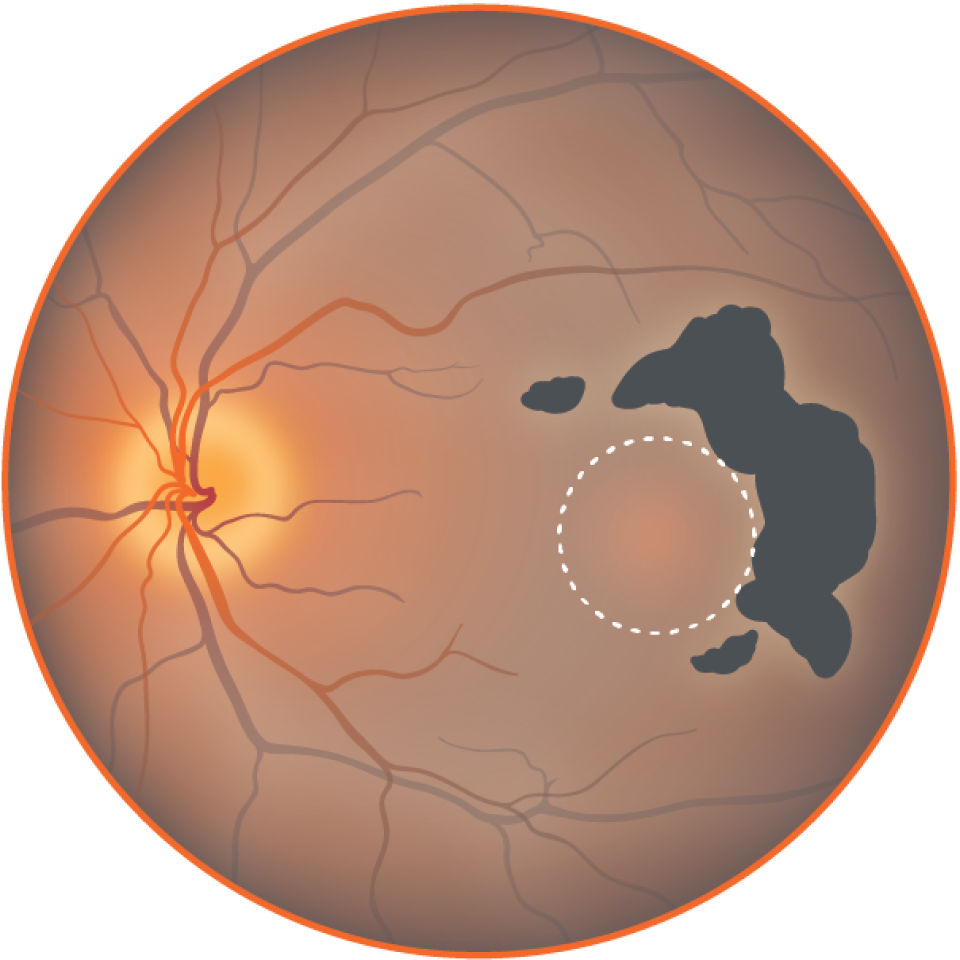
Loss of peripheral, low light vision.
Beginning to affect fovea, central vision
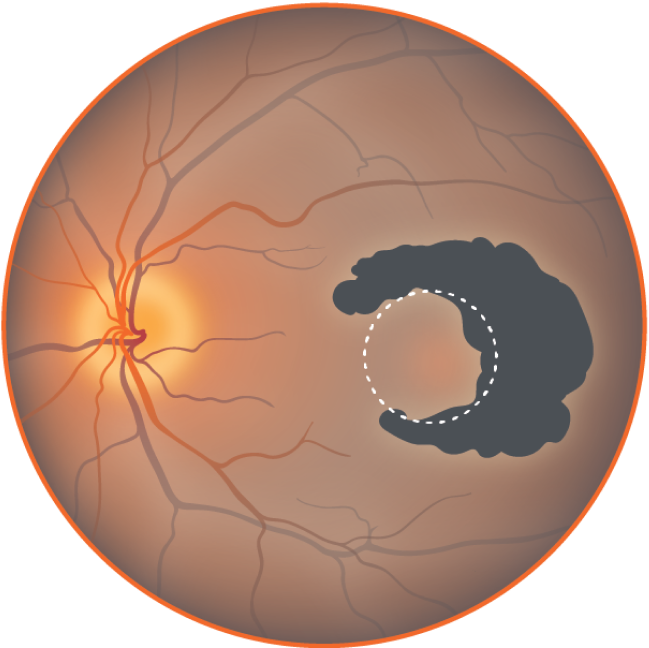
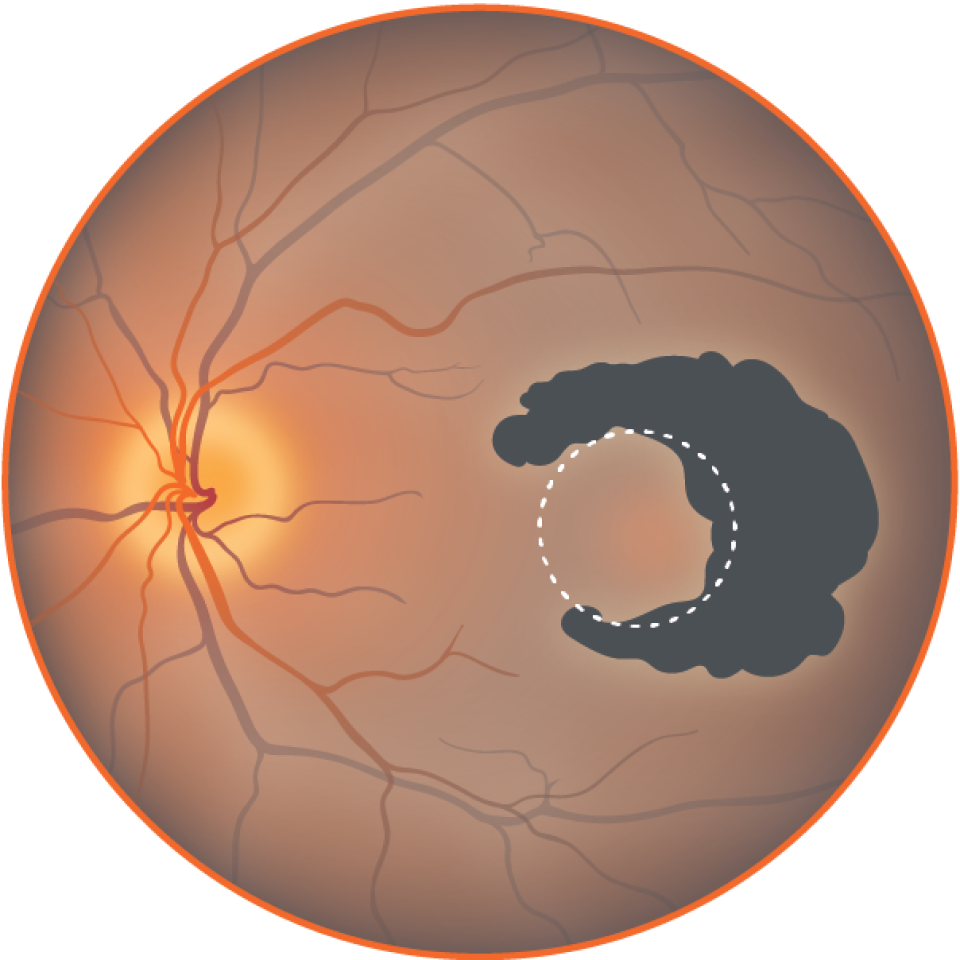
Loss of peripheral, low light vision; patches of lost central vision.
Severe central atrophy
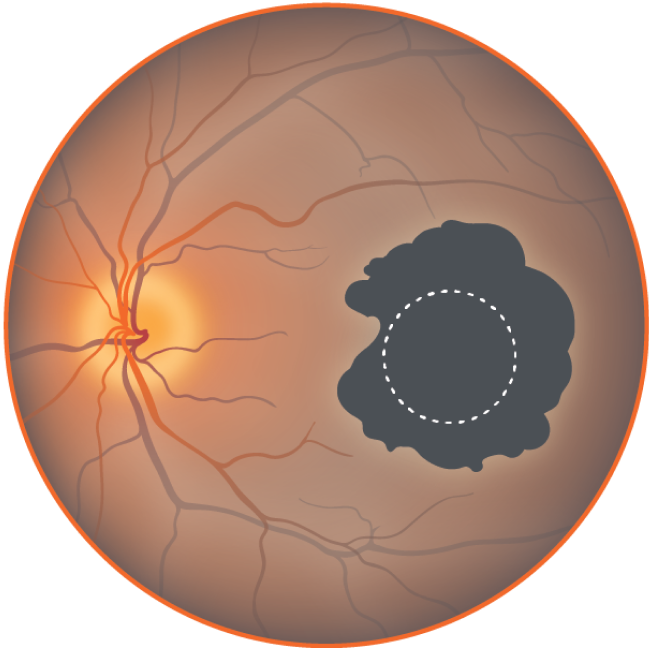
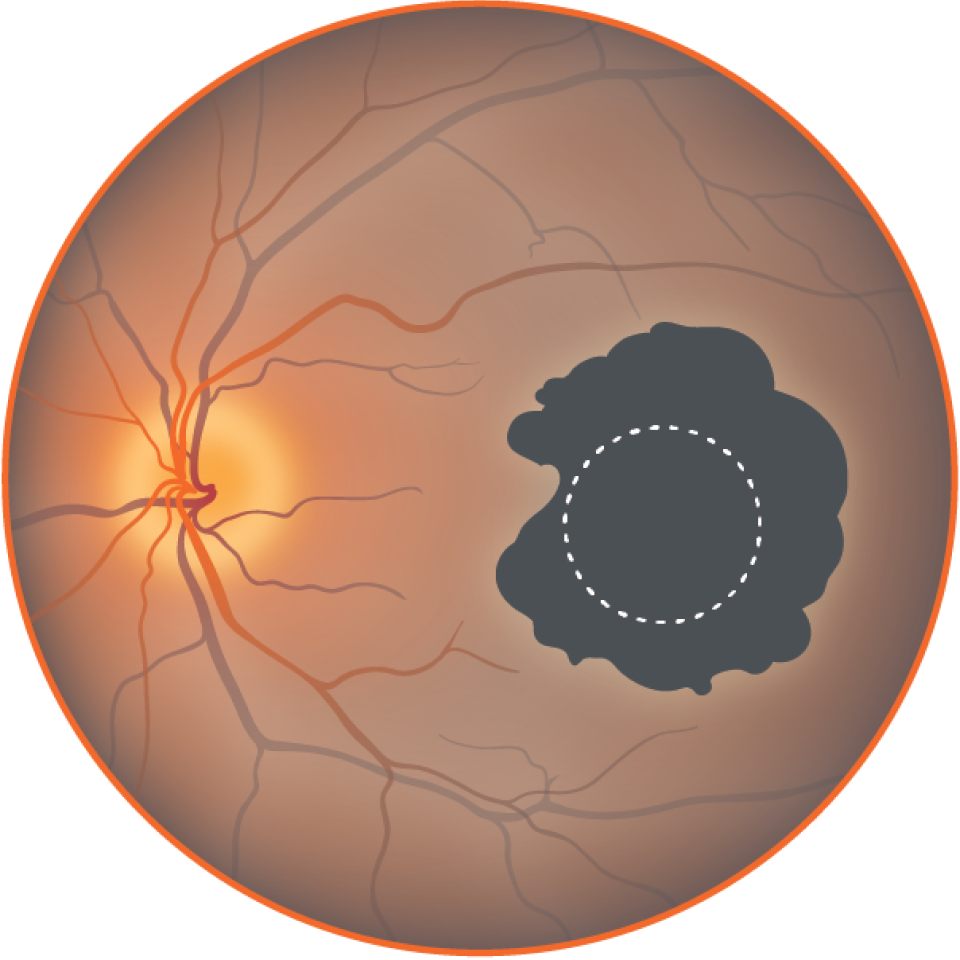
Loss of central vision leading to vision loss.
© 2023 Apellis International GmbH. All rights reserved.
How geographic atrophy impacts vision
As the drusen in the retina grow bigger and become more numerous, they might dim or distort the vision, especially when reading. As the disease progresses, blind spots in the centre of the vision may occur, eventually leading to loss of central vision.
The images below describe the experience of GA progression over time.*
1. Facial recognition

At diagnosis: Vision of a 70-year-old woman who has just been diagnosed with GA in both eyes. Her eyes have multiple lesions, making it difficult for her to see the faces of her loved ones.

2+ years: GA has progressed in both of the patient’s eyes. The faces of loved ones have become harder to see. Driving and other daily activities may become unsafe as lesions grow larger.
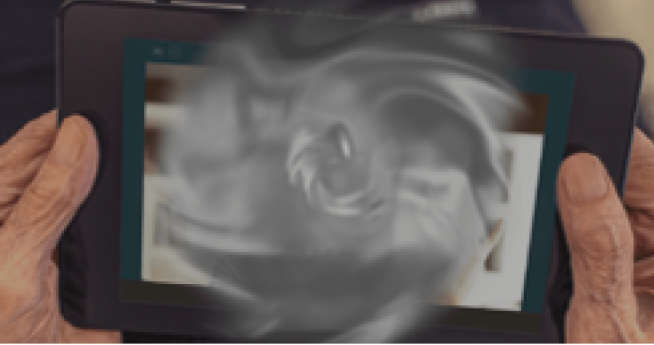
6+ years: Now, with increased progression in both eyes, the faces of loved ones, the ability to live independently, and overall quality of life have all been impacted by vision loss due to GA.
2. Daily activities

At diagnosis: Vision of a 70-year-old woman who has just been diagnosed with GA in both eyes. Her eyes have multiple lesions, making it difficult for her to read, for example, when shopping.

2+ years: GA has progressed in both of the patient’s eyes. Reading has become more difficult. Driving and other daily activities may become unsafe as lesions grow larger.

6+ years: Now, with increased progression in both eyes, reading, the ability to live independently, and overall quality of life have all been impacted by vision loss due to GA.
3. Eye chart

At diagnosis: Vision of a 70-year-old woman who has just been diagnosed with GA in both eyes. Her eyes have multiple lesions, making it difficult for her to see things, such as an eye chart.

2+ years: GA has progressed in both of the patient’s eyes. Letters have become hard to see. Driving and other daily activities may become unsafe as lesions grow larger.

6+ years: Now, with increased progression in both eyes, reading, the ability to live independently, and overall quality of life have all been impacted by vision loss due to GA.
*For illustrative purposes only. Vision impairment due to GA may vary.
Learn how you can optimise your environment and lifestyle to help adjust to GA and navigate any vision changes.
A closer look at wet age-related macular degeneration
Wet or neovascular age-related macular degeneration (nAMD) is the other advanced form of AMD. It develops due to the growth of abnormal blood vessels in the retina, which bleed and leak fluid that accumulates within the retina. This can cause distortion or loss of central vision.17
Access helpful resources
View the glossary section for further explanation of any unfamiliar terms used throughout this section and across the website.
References:
- Young RW. Surv Ophthalmol. 1987;31(5):291–306.
- EURETINA. Retinal diseases in Europe. 2017. Available at: https://euretina.org/resource/euretina-whitebook-on-prevalence-incidence-and-healthcare-needs-for-retinal-diseases-in-europe/ (accessed May 2023).
- Bear M, et al. Neuroscience: exploring the brain. 3rd edition. Library (Lond.); 2006.
- Macular Society. What is the macula? 2022. Available at: https://www.macularsociety.org/macular-disease/macula/ (accessed May 2023).
- Ardeljan D, Chan C. Prog Retin Eye Res. 2013;37:68–89.
- Macular Society. Age-related macular degeneration. 2022. Available at: https://www.macularsociety.org/macular-disease/macular-conditions/age-related-macular-degeneration/ (accessed May 2023).
- BrightFocus Foundation. Age-related macular degeneration: facts & figures. 2022. Available at: https://www.brightfocus.org/macular/article/age-related-macular-facts-figures (accessed May 2023).
- Gehrs KM, et al. Ann Med. 2006;38(7):450–471.
- Kaszubski P, et al. Ophthalmic Res. 2016;55(4):185–193.
- Wong WL, et al. Lancet Glob Health. 2014;2(2):e106–16.
- Fleckenstein M, et al. Ophthalmology. 2018;125(3):369–390.
- BrightFocus Foundation. What is geographic atrophy? 2023. Available at: https://www.brightfocus.org/macular/article/what-geographic-atrophy (accessed May 2023).
- Lindblad AS, et al. Arch Ophthalmol. 2009;127(9):1168–1174.
- Holz FG, et al. Ophthalmology. 2014;121(5):1079–1091.
- Sunness JS, et al. Ophthalmology. 2007;114(2):271–277.
- Boyer DS, et al. Retina. 2017;37(5):819–835.
- BrightFocus Foundation. Dry vs. wet age-related macular degeneration: what’s the difference? 2022. Available at: https://www.brightfocus.org/macular/article/dry-vs-wet-age-related-macular-degeneration-whats-difference (accessed May 2023).
EU-GA-2300004 June 2023